EBD Theory Becomes Practice At WellStar Paulding Hospital
In 2009, WellStar Paulding Hospital in Hiram, Ga., just outside Atlanta, was facing a dramatic growth in its local population, with an average 3.45 percent increase expected annually in Paulding County over the next five years. This reality pushed the need to consider replacing its existing 50-year-old, 32-bed hospital.
However, the decision came at a time when the organization was struggling financially, says Mark Haney, president of WellStar Paulding Hospital. Because of its commitment to the community and the potential for growth, WellStar decided to move forward. “We had a great culture,” Haney says, “and had been achieving strong metrics [for patient satisfaction and safety] once we started focusing on how to do things differently.” They decided to put that same focus on the design of its new building.
Getting it right
Project visioning began in 2009 and included a guiding principle sharply focused on safety. However, the project was quickly put on hold to await the outcome of the Affordable Care Act and how the legislation might affect the direction of its capital spending. In the meantime, WellStar continued its research on a new building by participating in The Center for Health Design’s (CHD) Pebble Project initiative.
Through the Pebble Project, Haney and his team visited peer facilities and heard from others on what they’d done on their own projects. “If I’d just researched all of this, I wouldn’t have soaked in all the knowledge that I did at this level,” Haney says. “The educational value of visual research by visiting other sites was extremely valuable.” He also says the effort allowed the team to think more innovatively and incorporate approaches into the building design that may not have been considered before.
Nine of Haney’s team members—including the medical director of the ER, the human resources director, finance director, chief nursing executive, and members of the design team—became certified in the Evidence-based Design Accreditation and Certification (EDAC) program, a credential offered by CHD to individuals who demonstrate a thorough understanding of how to apply an evidence-based process to the design and development of healthcare facilities. This knowledge, Haney says, gave the team a common language as they talked about design and helped define what a safe hospital would look like. It also made it easier to discuss issues and make decisions.
While this education was taking place, the hospital board was wrestling with some tough decisions. “The question was not whether to build, but how much to build,” Haney says. Concerned about capital spending, the decision was made to reduce the initial size of the hospital from 112 beds to 56, shelling in two floors to accommodate more beds as the population grew. The team was ready to move forward in fall 2010 on an eight-story, 295,700-square-foot hospital; a seven-story atrium that ties an existing medical office building (MOB) to a new four-story, 82,220-square-foot MOB and the new hospital; and a one-level, 120,000-square-foot precast parking deck.
WellStar made a commitment to the community that it would have its new campus completed by spring 2014, but its approved certificate of need from the state also defined a mandatory start date of Dec. 2, 2011 and completion date of July 2, 2014.
In order to open on time, the team fast-tracked the project by truncating the design phases into early-release packages, with general contractor Brasfield & Gorrie (Atlanta) beginning preconstruction work in March 2012 (six months before the construction documents were completed) and utilizing building information model and prefabrication to help expedite the process.
Applying the evidence
Filled with natural light, the new hospital features 56 private patient rooms with the ability to expand to 112, as well as 40 adult and pediatric emergency exam rooms, four surgical suites, decentralized nurses’ stations, administrative offices, and a café. According to Mary Lindeman, project manager for architecture firm CDH Partners (Marietta, Ga.), all decisions were guided by WellStar’s goal for safety—for patients and families, team members, the community, and the environment. This “safety first” approach had been WellStar’s focus in operating all of its hospitals and clinics.
And while the design team didn’t strictly follow CHD’s eight-step evidence-based design (EBD) process, it was tasked to look at the best available evidence to make design decisions that would produce the best outcomes. To do this, team members conducted an internal and informal literature review, with an emphasis on safety, compiling references and resources. Referencing the “Summary of the Relationships Between Design Factors and Healthcare Outcomes” by Roger Ulrich and Craig Zimring and an EBD checklist created by the SimTigrate Design Lab of the College of Architecture at the Georgia Institute of Technology for the Military Health System, the team implemented many design concepts that have been shown to achieve positive outcomes, including:
- Visually connected, decentralized nurse “perches” and teaming areas to play to the strengths of the decentralized approach of keeping caregivers closest to patients but avoiding the isolated/disconnected feeling users experience in decentralized units
- Same-handed patient rooms with the toilet room located on the headwall to keep patients from having to cross the room, with a continuous lighted handrail from the bed to the toilet to provide additional guidance
- Handwashing stations strategically located inside patient rooms between the door and patient, clearly visible as a reminder to wash hands and oriented such that the caregiver will not have his/her back to the patient
- Overhead lifts in all ADA/bariatric patient rooms, with all patient rooms configured to allow lifts to be easily installed in the future
- View windows with integral operable blinds at charting stations outside each patient room to provide increased visibility of the patient
- Nurse servers located outside each patient room to bring meds as close to the bedside as possible and minimize the potential for errors
- A family zone in the patient room that comfortably accommodates visitors and encourages family involvement in the care process
- Intuitive wayfinding from the street, with entry drives and a loop road to ease stress and anxiety, with the ED immediately visible and all entry points architecturally highlighted.
In addition, the hospital was designed to be a “no bump” building—all floor transitions are flush with the floor to eliminate trip hazards by removing thresholds and even small transition strips. Organizational and supply layouts are standardized so items are consistently in the same locations throughout the hospital to help staff find what is needed, when it’s needed. There’s also UV sterilization in all air handler units. “The first breath of air you take in this hospital has been treated to prevent infection,” Haney says.
Material choices and design decisions were also made to mitigate noise, such as acoustic panels in atriums, varied ceiling levels, and resilient flooring on patient floors. Situated seating groupings along corridors break up long, hard wa
lls and provide some absorptive quality, as well as additional choices for patients and family members to congregate outside of the patient room.
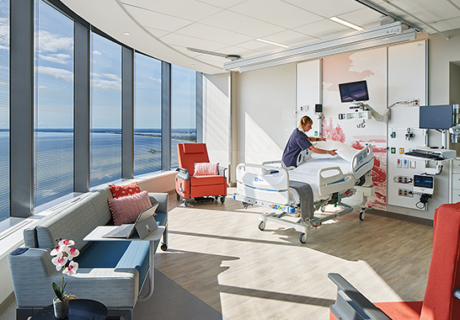
“Putting in lots of windows with chair space was my personal vision,” Haney adds. “I wanted to get patients out of the bed, give them a choice.” In patient rooms, a seating unit allows patients to have meals by the window, rather than in bed.
A worthwhile endeavor
In the end, the team was able to deliver the project on time and at budget, opening in April 2014. “We started off and finished with the same budget and opened on the day we set as a goal,” says Haney, who reports that several months after opening, the hospital is already beyond its fifth-year projections, with one noticeable problem so far. “We didn’t expect the ER to take off as fast as it did,” he says. “We probably should have built a bigger ER waiting room.”
As part of its Pebble Project participation, WellStar Paulding will conduct a post-occupancy evaluation on medication administration workflow, having already done some studies at its old facility. In the meantime, Haney is building the business case for expanding. “We have two floors shelled in that will give us 56 more beds,” he says, adding that the organization could probably use more than that.
Looking back at the process, Haney concludes that it was valuable to take the time to research and question the project’s direction. “If we’d stayed with a traditional approach, our outcome would not have been as unique and positive as it’s already proving to be,” he says.
Sara O. Marberry, EDAC, is a contributing editor for Healthcare Design and is based in Evanston, Ill. She can be reached at sara@saramarberry.com.
Project breakdown:
Completion date: April 2014
Total building area: 33 acres (site), 120,000 sq. ft. (parking deck), 295,700 sq. ft. (hospital), 82,220 sq. ft. (MOB)
Total construction cost: $94 million
Construction cost/sq. ft.: $266 (site/hospital/atrium/CEP), $105 (MOB), $22 (parking deck)
Owner: WellStar Health System
Architecture: CDH Partners
Interior design: CDH Partners
Engineering: Kimley-Horn (civil), Walter P Moore (structural), Perry Crabb Associates (MEP)
Construction: Brasfield & Gorrie LLC
Contractors: Art Plumbing, Inglett & Stubbs (electrical), R.F. Knox Co. (metal), Batchelor & Kimball (mechanical)
Carpet/flooring: Armstrong, Forbo, Shaw
Ceiling/wall systems: National Gypsum, USG
Doors/locks/hardware: Marshfield, Assa Abloy, Von Duprin, Ingersoll Rand, Architectural Builders Hardware, LCN
Equipment booms/surgical lights: Berchtold
Patient lifts: Arjo
Surfaces—solid/other: LG, Corian, Zodiac, Wilsonart